Researcher evaluates estrogen as therapy for knee osteoarthritis

LAWRENCE — More than 30 million Americans suffer from osteoarthritis of the knee, according to the Centers for Disease Control and Prevention. The degenerative joint disease, often caused by wear and tear, is a leading cause of disability in the U.S. Partly triggered by a breakdown in the fibrocartilage between the bones of the knee joint such as the meniscus, osteoarthritis results in pain, stiffness and less range of motion.
 Now, University of Kansas researcher Jenny Robinson is studying how estrogen may protect the menisci, the crescent-shaped pieces of fibrocartilage that absorb shock between the thighbone and shinbone. Her work is enabled by a one-year, $125,000 grant from the Center for Molecular Analysis of Disease Pathways, an NIH Center of Biomedical Research Excellence based at KU.
Now, University of Kansas researcher Jenny Robinson is studying how estrogen may protect the menisci, the crescent-shaped pieces of fibrocartilage that absorb shock between the thighbone and shinbone. Her work is enabled by a one-year, $125,000 grant from the Center for Molecular Analysis of Disease Pathways, an NIH Center of Biomedical Research Excellence based at KU.
“In general, osteoarthritis has a predisposition for women to experience it more than men, but it’s unknown why,” said Robinson, assistant professor of chemical & petroleum engineering. “Our hypothesis is that estrogen may be playing a role in the health of the meniscus and we can use estrogen potentially as a regenerative therapy. The easiest way to think about it is if you lose estrogen postmenopause — that’s when you have enhanced chances of osteoarthritis.”
Robinson said the meniscus has a complex mechanical structure, with some regions that are hard and others that are more like soft tissue. She dubbed these areas of the meniscus “microenvironments.”
“The meniscus is composed of fibrous cartilage known as fibrocartilage — an intermediate tissue between hard tissue like bone and soft tissue like cartilage,” she said. “It has regional properties throughout the disc including changes in the types of cell and the environment the cells live in. Some regions are closer to bone, and some are closer to soft cartilage.”
The KU researcher said chances of recovery from an injury to the meniscus depend on which region sustains damage.
“There are different ways to tear the meniscus,” Robinson said. “Depending on the location and severity of the tear, repair is limited. The part of the tissue that is like cartilage is avascular. Most tissue that is avascular doesn’t get the nutrients and oxygen needed to regenerate. Typically, if you get a tear in the avascular region you don’t heal. So, we’re trying to find out how to promote regeneration in this region.”
Using both in vitro and in vivo studies, Robinson and her collaborators hope to determine how estrogen acts on meniscal fibrochondrocyte transcriptional changes, cell type, extracellular matrix production and response to mechanical signals.
“We’re looking at what estrogen does to human cells in a cell culture dish — how do we change the genes being transcribed, and which genetic material is being increased or decreased due to estrogen?” Robinson said. “What are the changes to proteins and sugars these cells are making — that’s what these cells do to create a healthy environment.”
Robinson plans to test estrogen treatments alone and in combination with changes to the mechanical microenvironment in 2D and 3D models.
She said the aim of the basic science is eventually to develop targeted, estrogen-based therapies to treat people who otherwise would cope with osteoarthritis for the rest of their lives.
“The goal here is to make an off-the-shelf material, specific for sex and age, that a surgeon could implant into the knee instead of or after performing a meniscectomy,” Robinson said. “I’ve talked with orthopedic surgeons who hope for something we could inject into the knee and it would interreact with tissue, provide support and give off signals for repair. The hope is that you’d get full regeneration. Depending on your status when you got this treatment, this therapy could inhibit osteoarthritis when you’re young or, if you already have osteoarthritis, reduce the rate of further degeneration.”
According to Robinson, the results of her study on the meniscus could influence future treatments for parts of the body beyond the knee joint.
“What we find in the meniscus will likely be analogous to fibrocartilages in other joints including the shoulder, spinal discs and jaw,” she said.
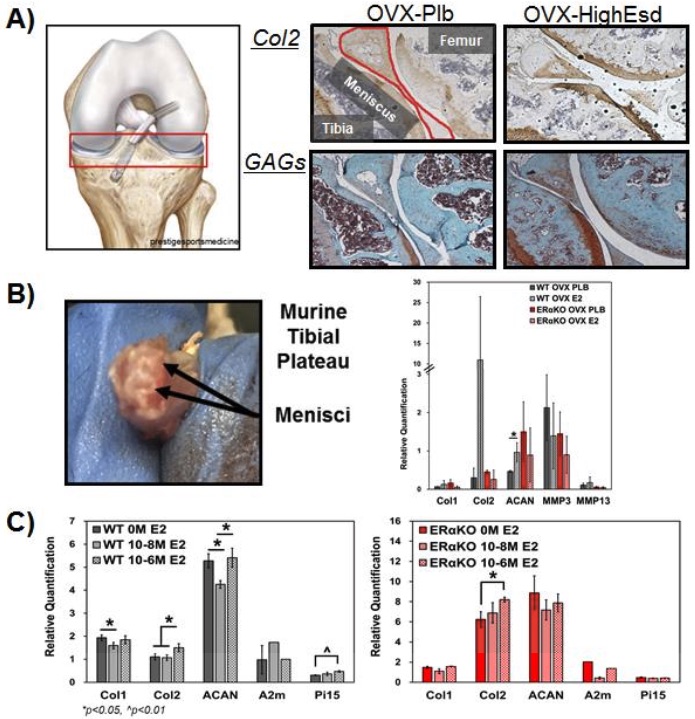
Top image: Stock photo, credit Pixnio.com.
Bottom image: Estrogen promotes increase in cartilaginous markers. Estradiol treatment in ovariectomized mice resulted in increase in collagen type II (Col2) and charged glycosaminoglycan (proteoglycans-SafO) histological staining (A) an increase in Col2 and aggrecan gene expression in WT but not estrogen receptor alpha knock out (ERαKO) mice (B) Estradiol treatment to meniscal fibrochondrocytes isolated from female WT and ERαKO mice resulted in increased gene expression of Col2 (C). n=6, *p<0.05, ^p<0.01. Credit: Assistant Professor Jenny Robinson, University of Kansas.